
Home - Medical Grade Plastics Applications - Implantable PEEK Film and Components in Cardiovascular Surgery
Home - Medical Grade Plastics Applications - Implantable PEEK Film and Components in Cardiovascular Surgery
The cardiovascular system spans the entire body, supported by the constant pumping of the heart. In effect, the cardiovascular system is the body’s supply chain, and if it fails, the rest of the body does as well. Medical science and engineering have placed much focus on protecting and repairing the heart, even going as far as ‘backing it up’ with an implantable defibrillator. Modern defibrillators can react to arrhythmias instantly, correcting the pace and enabling the heart to function properly. These defibrillators can deliver electrical shocks of varying intensity when the heart is threatened with sudden failure. Similarly, pacemakers are also implanted to help adjust the pacing, or beating rhythm of the heart.
The implantable cardioverter-defibrillator (ICD) remains a frontline treatment choice for patients at risk of cardiac death, but additional treatment options are needed for patients who have already suffered a myocardial infarction. During a myocardial infarction, the heart muscle sustains damage, and tissue death and scarring are expected. Prognosis depends mainly on the extent of tissue death and the resulting scarring.
The left ventricle is often hit hard by myocardial infarction, and much of the scarring is located there following a heart attack. Extensive scarring can change the shape of the ventricle, affecting its volume and ability to facilitate circulation. Until recently, the only way to correct this was with Surgical Ventricular Restoration (SVR). SVR, though, comes with sizeable risks. For one, the heart has to be stopped during the procedure and cardiopulmonary bypass employed, which is a risky maneuver. It can lead to postperfusion syndrome, hemolysis, capillary leak syndrome, blood clots, embolisms or rapid exsanguination if a bypass line fails. Further, SVR requires the surgeon to make several incisions into the heart muscle to excise the scar tissue, which can lead to further damage if a mistake is made.
Fortunately, recent advances in medical engineering have produced a less invasive and less complicated alternative to SVR, and this is one area where PEEK polymer comes in. The SVR alternative is a procedure developed by BioVentrix, a medical device manufacturer, and is known as Less Invasive Ventricular Enhancement (LIVE). LIVE has already been performed on more than 50 patients successfully, though it has only been available for a short time.
During a LIVE procedure, a pair of anchors, connected by a PEEK tether, are positioned adjacent to left ventricle scarring. The internal anchor is placed percutaneously and over the scar tissue. The external anchor is positioned on the left ventricle epicardium. The PEEK tether connects the two anchors, provides traction and ensures the anchors remain in alignment. Together, the anchors and tether help position the left ventricle wall, and restore proper circulation.

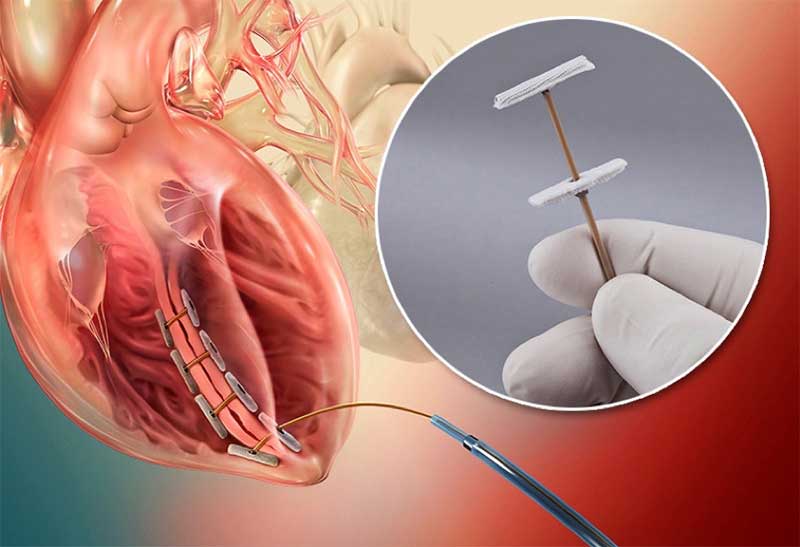
Additional cardiovascular applications include a variety of connectors and components used to produce defibrillators and pacemakers. PEEK is an attractive material choice for several reasons, including:
PEEK is completely inert in the body, so it can serve as a reliable component in a long-term solution. As cardiac implants are expected to last for many years, biocompatibility is an important attribute.
2. Optimal strength
The LIVE procedure demands materials that can withstand the constant movement exerted by the heart’s beating. PEEK’s strength has been proven in some of the most demanding applications imaginable, making it an ideal option for LIVE.
3. Viability in less invasive, less traumatic procedures
PEEK and PAEK can be fabricated in extremely small sizes, so they can be used to produce very small medical components. PAEK’s processing versatility allows components to be manufactured down to extremely small dimensions, which makes it a strong choice for less invasive procedures, and PEEK’s role in the LIVE procedure means surgeons have an alternative to cardiopulmonary bypass and risky heart incisions. PEEK can be produced in thicknesses of only .040 in. and be fabricated to rectangular shapes just .040 in. wide x .065 in. deep x 12 in. long.
4. Tight engineering tolerances
PEEK and PAEK components can be easily fabricated so that critical components and connectors can be produced to extremely tight tolerances. Alternative materials like Polysulfone have also been utilized in some of these applications.
Cardiovascular surgery demands precision and long-term viability. PEEK and PAEK components are ideal in providing both, and can serve in critical roles for innovative cardiovascular treatments.